Your Behavioral Health Ecosystem
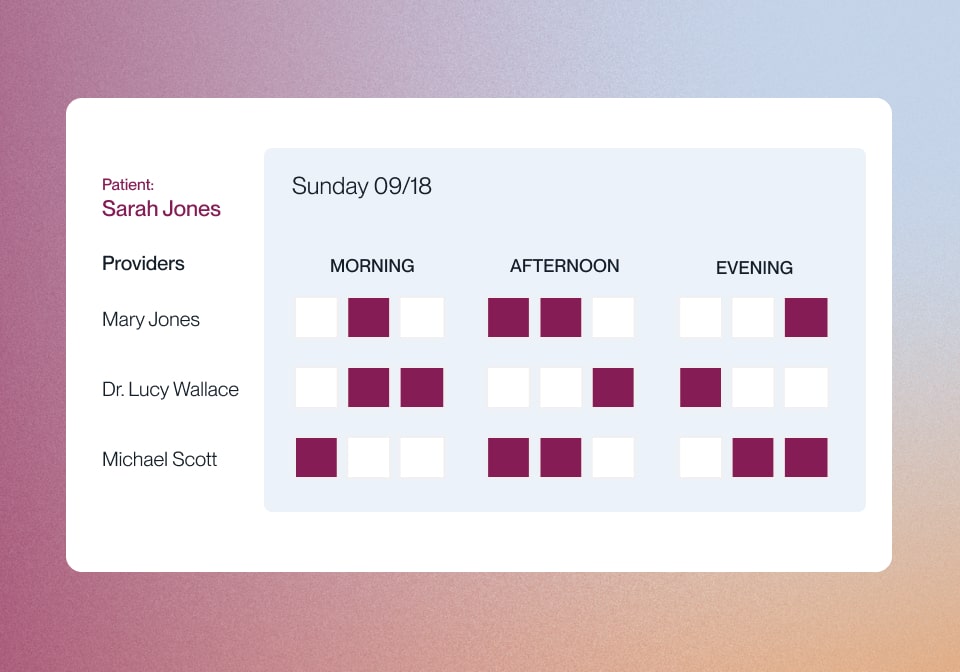
With Lucet, optimize your health plan members’ access to behavioral health and achieve better outcomes at a lower cost.
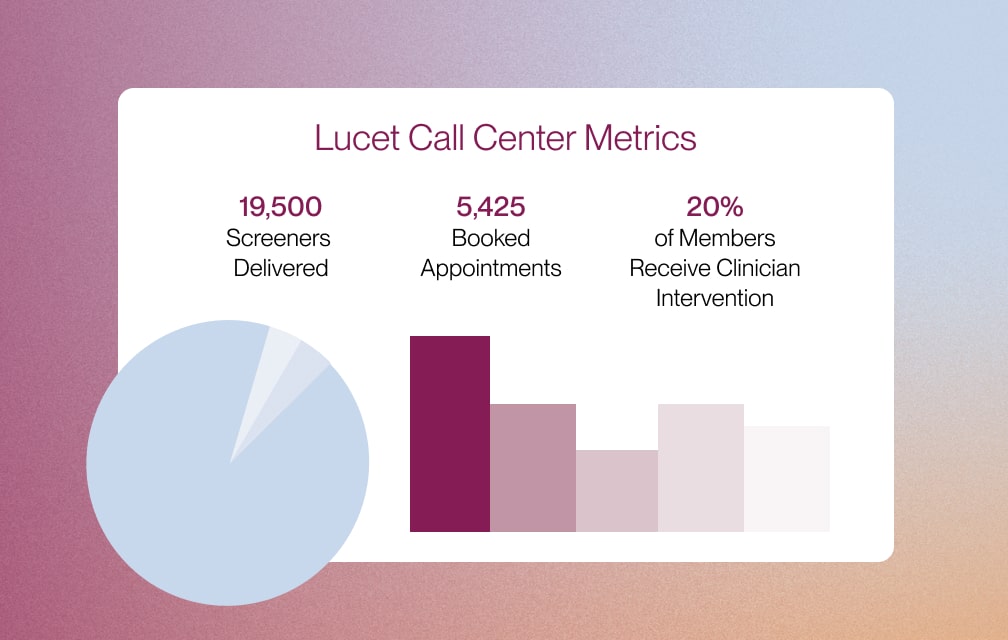
We are the country’s leading behavioral health optimization company—removing complexity and providing the infrastructure for health plans and providers to optimize access to behavioral healthcare through quality, speed, and outcomes.
How We Optimize Your Behavioral Health Ecosystem
Our NavConnect™ Platform Offers:
Meet Lucet. We are the only company delivering real-time behavioral health optimization.
Learn MoreCore Services
Lucet serves those who are affected by mental illness and impacted by trauma. We offer the most cost-effective care, from integrated care coordination to specialty clinical programs.