Rethinking Behavioral Health’s First Call
Behavioral healthcare has a problem: most health plan members seeking care face significant hurdles prior to ever being connected.
Today, when a person makes the decision to seek mental health care, many do not know where to start. For those searching their health plan’s online directory of providers. This list of providers is often outdated and members have no guidance regarding which provider or type of care is right for their needs. Members contacting their health plan are often provided with a similar list, and are then on their own to cold-call providers to find the right one. Wait times to schedule a first available appointment can be as long as three months. Over half of adults with mental illness never make it to care.
It’s crucial we rethink this first point of contact. The initial conversation that health plans have with a member should act as a switchboard that launches them on the most direct, efficient and accurate path to improved mental health outcomes. This requires evaluating which care is the right match for member needs, connecting them to it and escalating high risk members to care quickly.
Universal screening and connecting to care at first contact
At Lucet, we ensure that health plans make the most of that first call. Our care navigators greet members who call into our Care Center, then guide each one through a standardized risk screening and matching process using our technology platform. Every member across the acuity spectrum receives the same screening, which has been backed by nearly three decades of clinical research. With this knowledge, care navigators can immediately determine a member’s risk level and either warm transfer them to an appropriate clinician or schedule a first appointment with a covered provider—all in one call.
Using this universal screening model, Lucet saw a massive 152% increase in the number of members identified as at-risk who were triaged to a clinician for further assessment and safety planning. The Lucet technology platform has proven critical to effectively implementing a solution across the acuity spectrum. It allows care navigators to both inform low-risk members about direct scheduling and identify at-risk members who were previously overlooked. In fact, up to 5% of callers to our Care Center were members asking about benefits who were identified as needing risk escalation in the same phone call. When implemented at scale for all members, this differentiator ensures we can identify the need for immediate intervention with a clinician and potentially avert a catastrophic event.
Uncovering overlooked high-acuity members
In an analysis across 5,000 members screened by our Care Center, 21% of total members were low acuity, 47% were moderate and 32%—a third of the entire population—were identified as high acuity (based on our Behavioral Health Index). As a significant number of members reaching out are screening as high risk, establishing a connection and appropriately triaging within the first call is crucial. Standardized risk screening gives health plans the ability to identify all patient needs, especially the high acuity population, at the onset of their care to route them to the right treatment as quickly as possible.
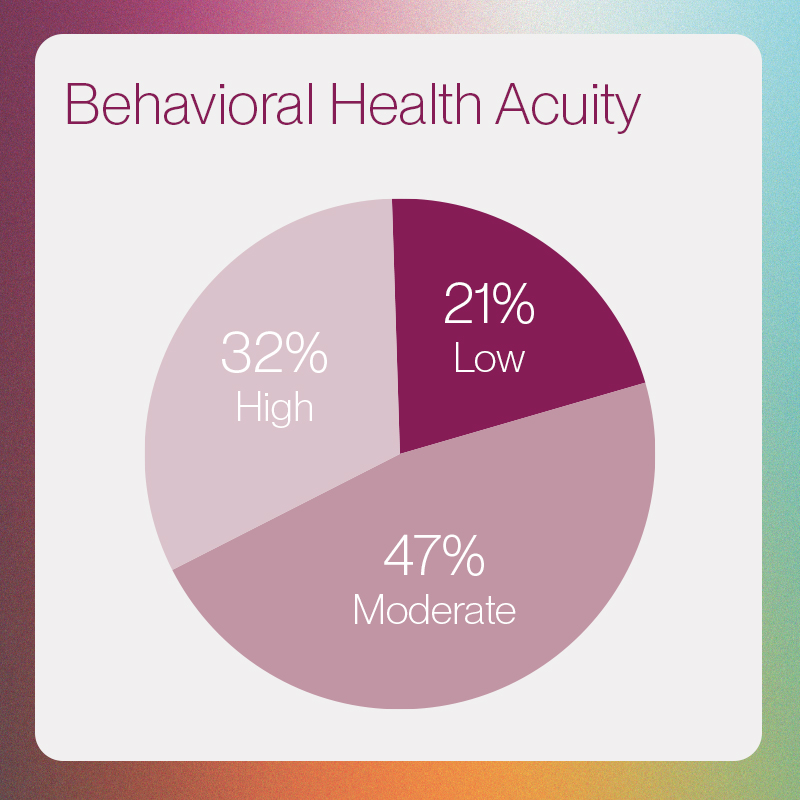
Health Index (BHI) in Lucet Care Center
Over time, data gathered from these clinically informed screeners provide health plans with a holistic view of behavioral health needs across their total member population. This enables plans to evaluate demand and address provider supply issues across their network and meet total member population needs.
Escalating high-risk patients to clinical staff
In our analysis, 15% of all calls to our Care Center needed immediate clinician intervention. Interventions are required immediately for these members, and include face-to-face evaluation within one hour for imminent, life-threatening situations and within six hours for non-life-threatening situations.
To manage the needs of these members, Lucet maintains a team of licensed clinical staff who are available 24/7, 365 days of the year. For escalated members, these clinicians conduct a complete clinical screening, ensure member safety and coordinate with the referred provider to ensure follow-up screenings and treatment success.
As a result of a more effective first call, Lucet has been able to connect 26% more members to care, and has demonstrated 40% improvement in outcomes.

connections to care
If you’re a health plan interested in transforming your behavioral health first call or learning about Lucet’s screening and escalation process, contact lucetsales@lucethealth.com.
Leza Ogren is the Vice President of Clinical Operations at Lucet, The Behavioral Health Optimization Company.



